In Case 20 of the 2017.2 KFP you visit Betty, an 80 year old who presents with acute upper back pain that happened while gardening. She has a history of late menarche and early menopause, had 3 years of HRT before ceasing. Spinal Xray was performed.
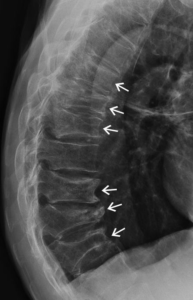
What are the abnormalities present in this Xray? (list 5)
- Kyphosis
- Wedge compression fractures
- Vertebral body osteophytes
- Degenerative changes of the intervertebral disc spaces
- Endplate sclerosis
What is the most likely diagnosis for this presentation? (list 1)
- Thoracic vertebral crush fractures secondary to osteoporosis
What are the most important initial investigations to conduct? (list 3)
- Bone Mineral Density
- Calcium
- Vitamin D
From https://www.racgp.org.au/download/Documents/Guidelines/Musculoskeletal/osteoporosis-guidelines.pdf
Measure bone mineral density (BMD) by dual energy X-ray absorptiometry (DXA) scanning on at least two skeletal sites, including the lumbar spine and hip, unless these sites are unsuitable (eg hip prosthesis).
What are the non-pharmacological strategies that would assist in ongoing management? (list 6)
- Exercising regularly within limits
- Smoking cessation
- Alcohol minimisation
- Adequate calcium intake – Aim for a minimum of 1000 mg/day
- Adequate but safe exposure to sunlight as a source of vitamin D
- Maintenance of a healthy weight and body mass index
From https://www.racgp.org.au/download/Documents/Guidelines/Musculoskeletal/osteoporosis-guidelines.pdf
Promote the following important lifestyle choices for all postmenopausal women and men over 50 years of age:
• Adequate calcium and protein intake
• Adequate but safe exposure to sunlight as a source of vitamin D
• Maintenance of a healthy weight and body mass index
• Cessation of smoking
• Avoidance of excessive alcohol consumption
From https://www.racgp.org.au/download/Documents/Guidelines/Musculoskeletal/osteoporosis-algorithm.pdf
Leisure walking, swimming and cycling do not improve bone density. Prescribe regular, varied, high-intensity resistance
training and progressive balance training (Recommendation 11 A). High-impact activities should be avoided by individuals
at high risk of fracture. Avoid forward flexion and twisting in vertebral osteoporosis. Programs should be individualised and
may require supervision.
RACGP Feedback – Case 20
This case focused on an older female patient presenting with acute onset of upper-back pain. Candidates were required to interpret the lateral spinal X-ray that was provided and identify the diagnosis of osteoporosis and provide appropriate initial investigations. These elements of the case were covered well by the majority of candidates; however, the final question requested non-pharmacological strategies to assist in ongoing management. This was not answered as well, with candidates providing either pharmacological advice or nonspecific advice, such as the commencement of vitamin D supplementation.
RACGP Conclusion on Technique
As outlined above, there are some common themes and key issues to consider when approaching the KFP exam:
- The KFP exam is not a simple short-answer paper. You must answer the question in the context of the clinical scenario provided, utilising all of the information provided. Read the scenario at least twice.
- Keep your answers succinct.
- Only provide the number of answers requested. Review your answer – have you created a list rather than one answer per line? If so, you will be penalised for extra answers.
- Always read the question at least twice and, after you answer, check that you have answered the actual question asked.
- Be specific in your answers, whether in the investigations being ordered or the treatment you are prescribing. Non-specific answers will not score or will attract a much lower score.
- General answers such as ‘educate’, ‘refer’, ‘reassure’ or ‘review’ do not score without specific detail. For example, providing a review timeline and details about the specialist to whom you are referring (along with degree if urgency, if appropriate) may score marks if relevant to the scenario and question.
- Be aware of clinical guidelines and any important changes or additions to treatments. If guidelines change very close to the exam, the marking keys are adapted to consider the original and the new guidelines so candidates are not penalised if they have not seen a guide published close to the exam sitting.
- Access the practice exams provided after enrolment closes and utilise the RACGP assessment resources provided for candidates.
References
- https://www.racgp.org.au/osteoporosis
- https://www.racgp.org.au/download/Documents/Guidelines/Musculoskeletal/osteoporosis-guidelines.pdf
- https://www.racgp.org.au/download/Documents/Guidelines/Musculoskeletal/osteoporosis-algorithm.pdf







