Geoff, 75, presents with sudden onset painless visual disturbance over 24 hours in his right eye which started on waking, on a background of poorly controlled T2DM and HTN, Hyperlipidaemia. On examination VA is reduced to 6/60 and not improved with 1mm pinhole, you note a relative afferent pupillary defect.
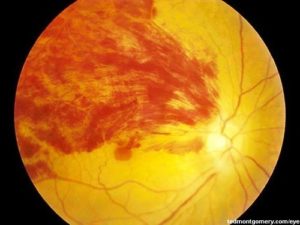
What is the most likely initial diagnosis?
- Central Retinal Vein Occlusion
What are the causes / associations of this condition?
- Age
- Hypercoaguable state
- Atherosclerosis
- Retro bulbar compressive lesions
- Anaemia
- Diabetes
- Glaucoma
- Hyperlipidaemia
- Hypertension
- Smoking
- Obesity
- Sarcoidosis
- Behcets Syndrome
What the key features of history of this condition?
- Sudden loss of central vision in one eye
- Unilateral
- Painless
- Blurred vision (if macular involvement)
- Sudden
- +- field defect
- Probable history of CVD risk factors
What are the key features of examination in this condition?
- Marcus-Gunn pupil if ischaemic
- VA variable depending on severity and duration and macula involvement
- Vision not improved with 1mm pinhole
- Stormy sunset appearance
- Multiple retinal haemorrhages
- Retinal Vascular dilatation
- Optic disc oedema
What Investigations would you consider to identify the most likely underlying causes?
- Fasting BSL
- HBA1c
- Blood pressure
- Lipids
- FBC
- ECG
- UEC
- LFT
What is the most important initial feature of management in this condition?
- Referral to Ophthalmology
What are the key features of general approaches to long term management in this condition?
- Treat underling cause
- Screen for risk factors and treat
[wpforms id=”7496″ title=”false” description=”false”]







