


RACGP KFP 2016.1.8 – Letifa has Gestational Diabetes
Letifa, a 21 year old woman presents in December at 26 weeks gestation of her first pregnancy. She had her initial bloods and ultrasound done at her old practice before she moved to the area. She reports She was overweight before her pregnancy with a BMI of 32. She is Muslim and often wears head scarfs like a hijab and sometimes covers her arms and legs. She takes no medication or allergies. Her blood pressure is 122/74. She is rhesus negative.
RACGP KFP 2016.1.6 – Julie has pain in the leg
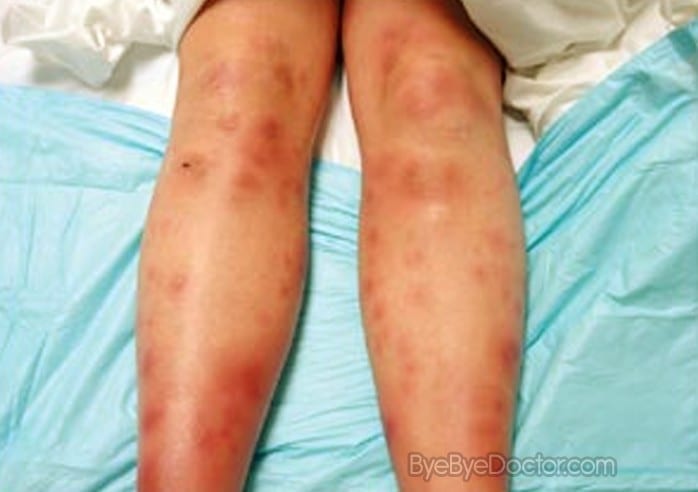
Julie, a 29 year old women presents to you with a pain in the back of her leg which came on whilst playing touch football 1 week ago. She wasn’t going to play this game as she has been fighting a sore throat for the past 2 weeks and is generally more fatigued especially over the past 3 months due to chronic diarrhoea and lower abdominal pain which she assumed would clear eventually.
This hamstring pain has happened once before at the end of the season last year, but resolved over 4 weeks. She is strictly compliant with levlen ED and takes paracetamol 1g qid prn. Whilst you are examining her legs you notice some red lumps on her shins as shown in picture 1.

RACGP KFP 2016.1.4 Bryan has facial pain
Bryan, a 32 year old man presents to your rural hospital around 6am on a Sunday with an extremely severe stabbing pain in his face on the right side. It has been present for 45 minutes. He reports he has now had 7 attacks like this around the same time every day over the past few weeks but usually only last 15 minutes. He smokes and drinks quite heavily most weekends. He has no other medical history and takes no regular medications.

RACGP KFP 2016.1.2 – Acute back pain
Wonda, a 62 year old women presents to you with acute onset of lower back pain. She ranks the pain as an 8/10. She was helping her daughter move house yesterday and was moving some books from a car the same day it came on. The pain is better lying down and worse bending forwards. This is not her first episode of acute low back pain, it happens at least twice a year.
She has a background of hypertension, asthma that is worsened by mobic and she is overweight and putting on more. Her medications include symbicort 200/6 bd, ventolin prn, perindopril 10mg and indapamide 1.25m and panadol regularly. She requires courses of prednisolone on average 1-2 times a year. She is an ex-smoker, recently quit.
What are the most likely differential diagnosis? List 3
- Paraspinal muscular strain
- Facet joint pain
- Lumbar vertebral disc prolapse
- Lumbar vertebrae crush fracture
RACGP – There were a broad range of answers provided by candidates, highlighting again the need for candidates to look at the most like differential diagnoses. Not just listing all causes of back pain or providing answers relevant to the board clinical context. Listing causes of back pain in a male patients such as metastatic prostate cancer would obviously not have scored.
What further history do you want to know? List 4
- Radiation down her legs
- Weakness in legs
- Sensation changes in legs
- Bladder dysfunction
- Bowel dysfunction
GPCC – This question wasn’t explicitly mentioned as being in the Public Exam Report. Our take on answering this question was to differentiate between the broad severity categories – Category A – D as described in Murtaghs.
Case continued… Wonda reports the pain is localised in her lower back and she denies radiation, bowel or bladder changes and no neurological symptoms. You performed an xray to check for crush fractures which was normal.
What are the initial management steps in Wonda? List 4
- Movement as tolerated (2)
- Analgesia panadeine forte 1g/60mg qid prn (2)
- Referral to physiotherapy for preventative exercises (2)
- Bone mineral density scan (2)
- Heat pack (1)
- Review in 1-2 weeks (1)
GPCC – no marks would be given for saying panadol, as the stem already indicates she is taking this. Likewise NSAIDs in asthma and her medication combination would not be ideal and her response to Mobic would make this a poor choice.
RACGP – In managing the condition the question asked about the next steps after investigations. In the KFP paper candidates are requested to provide a specific number of answers, in this case there was a request for four answers. If candidates provide extra responses above this then there is a penalty for each answer above the four answers. Answers are meant to be short, and one answer per line. No request was made to explain, expand or justify the management steps given. In doing any of these candidates risk being penalised for extra responses.
RACGP Feedback
This case revolves around a 62yr old woman with acute onset of back pain after moving some books from a car. The case focuses on the ability to assess and manage a simple musculoskeletal injury whilst taking into consideration comorbidities of asthma and hypertension.
There were a broad range of answers provided by candidates, highlighting again the need for candidates to look at the most like differential diagnoses. Not just listing all causes of back pain or providing answers relevant to the board clinical context. Listing causes of back pain in a male patients such as metastatic prostate cancer would obviously not have scored, It is important exam technique to ensure you read the scenario, and identify the key information about the patient, such as age and gender.
In managing the condition the question asked about the next steps after investigations. In the KFP paper candidates are requested to provide a specific number of answers, in this case there was a request for four answers. If candidates provide extra responses above this then there is a penalty for each answer above the four answers. Answers are meant to be short, and one answer per line. No request was made to explain, expand or justify the management steps given. In doing any of these candidates risk being penalised for extra responses. It is good exam technique to review the answers and if you have used phrases/words such as ‘for example’, ‘because’, or ‘and’ or even need to use commas then the answer is most likely to contain extra responses and therefore attract penalties.
GPCC Feedback
This question should be well within your studied topics, should have been encountered regularly and should be a question that scores well.
Further reading:
- https://www.nps.org.au/australian-prescriber/articles/managing-low-back-pain-in-primary-care
- eTG good
- Murtaghs good , particularly on the categories, red flag exclusion, inclusion within the Masquerades
AFP Articles Tagged with Topic “Aged care”
- General practice encounters with patients living in residential aged care facilities from Volume 44, No.4, April 2015
- Models of general practitioner services in residential aged care facilities from Volume 44, No.4, April 2015
- Minimising psychotropic use for behavioural disturbance in residential aged care from Volume 44, No.4, April 2015
- Advance care directives in residential aged care from Volume 44, No.4, April 2015
- Antibiotic use in residential aged care facilities from Volume 44, No.4, April 2015
- Pain management in residential aged care facilities from Volume 44, No.4, April 2015
- CARE-PACT: a new paradigm of care for acutely unwell residents in aged care facilities from Volume 44, No.4, April 2015
- Nursing home patients from Volume 44, No.4, April 2015
- Eye care in the elderly from Volume 43, No.7, July 2014
- Reducing falls risk in older people from Volume 43, No.4, April 2014
- Core palliative medicines from Volume 43, No.1, January/February 2014
- Older people driving safety from Volume 42, No.5, May 2013
- Time poor from Volume 42, No.5, May 2013
- SPECT studies from Volume 42, No.3, March 2013
- Prescribing for older people with cri from Volume 42, No.1, January/February 2013
- Reflections on wisdom from Volume 41, No.12, December 2012
- Chronic problems from Volume 41, No.12, December 2012
- Medication list from Volume 41, No.12, December 2012
- Falls prevention from Volume 41, No.12, December 2012
- Dementia update from Volume 41, No.12, December 2012
- CKD in the elderly from Volume 41, No.12, December 2012
- Clinical challenge from Volume 41, No.12, December 2012
- Overactive bladder syndrome from Volume 41, No.11, November 2012
- Bone scans from Volume 41, No.9, September 2012
- Managing undernutrition in the elderly from Volume 41, No.9, September 2012
- Dementia and driving from Volume 41, No.4, April 2012
- Fitness to drive from Volume 41, No.4, April 2012
- Vitamin D and the musculoskeletal health of older adults from Volume 41, No.3, March 2012
- Anticholinergic and sedative medicines from Volume 41, No.1, January/February 2012
- Frontotemporal dementia from Volume 40, No.12, December 2011
- Fitness to drive forms from Volume 40, No.11, November 2011
- Lower urinary tract symptoms from Volume 40, No.10, October 2011
- Asymptomatic bacteriuria from Volume 40, No.10, October 2011
- Heatwaves and the elderly from Volume 40, No.8, August 2011
- Letters to the editor from Volume 39, No.11, November 2010
- AFP in Practice from Volume 39, No.10, October 2010
- Aging and sexuality from Volume 39, No.10, October 2010
- Androgen deficiency in the aging man from Volume 39, No.10, October 2010
- Bones beyond 70 from Volume 39, No.10, October 2010
- Clinical challenge from Volume 39, No.10, October 2010
- Clinical trials in general practice from Volume 39, No.10, October 2010
- Early dementia from Volume 39, No.10, October 2010
- Older patients from Volume 39, No.10, October 2010
- Prescribing in the elderly from Volume 39, No.10, October 2010
- Substance misuse from Volume 39, No.10, October 2010
- Quality use of medicines in residential aged care from Volume 39, No.6, June 2010
- General practice registrars – attitudes of older patients from Volume 39, No.6, June 2010
- Older patients and GP registrars from Volume 38, No.11, November 2009
- Letters to the editor from Volume 38, No.10, October 2009
- Dementia from Volume 38, No.8, August 2009
- Weight loss and malnutrition in the elderly from Volume 38, No.7, July 2009
- Persistent hyperkalaemia from Volume 38, No.5, May 2009
- Upper cervical spine injuries from Volume 38, No.1, January/February 2009
AFP Articles Tagged with Topic “Orthopaedics “
- Septic arthritis in children from Volume 44, No.4, April 2015
- Heel pain: a practical approach from Volume 44, No.3, 2015
- Editorial: Foot problems from Volume 44, No.3, 2015
- Exercise in pregnancy from Volume 43, No.8, August 2014
- Predicting recovery from whiplash injury from Volume 43, No.8, August 2014
- Osteopathy from Volume 43, No.4, April 2014
- Hip pain in young adults from Volume 43, No.4, April 2014
- Sports-related concussion from Volume 43, No.3, March 2014
- Painful swollen wrist from Volume 42, No.5, May 2013
- Tendon injuries from Volume 42, No.4, April 2013
- Extrapulmonary tuberculosis from Volume 42, No.4, April 2013
- MRI of the knee from Volume 41, No.11, November 2012
- Making sense of MRI of the lumbar spine from Volume 41, No.11, November 2012
- Back pain with lower limb paresis from Volume 41, No.10, October 2012
- Clubfoot from Volume 41, No.5, May 2012
- Sprains and strains from Volume 41, No.4, April 2012
- Meniscal tear from Volume 41, No.4, April 2012
- Shoulder injuries from Volume 41, No.4, April 2012
- Cervical spine from Volume 41, No.4, April 2012
- Hands, fingers, thumbs from Volume 41, No.4, April 2012
- Initial assessment of the injured shoulder from Volume 41, No.4, April 2012
- The Ottawa knee rules from Volume 41, No.4, April 2012
- Clinical challenge from Volume 41, No.4, April 2012
- Bennett fracture dislocation from Volume 40, No.6, June 2011
- Anterior shoulder dislocation from Volume 40, No.3, March 2011
- Mallet finger from Volume 40, No.1, January/February 2011
- Clinical challenge from Volume 40, No.1, January/February 2011
- Skier’s thumb from Volume 39, No.8, August 2010
- Musculoskeletal pain – presentations to general practice from Volume 39, No.6, June 2010
- Letters to the editor from Volume 39, No.4, April 2010
- Charcot osteoarthropathy of the foot from Volume 39, No.3, March 2010
- Slipped upper femoral epiphysis in children – delays to diagnosis from Volume 39, No.3, March 2010
- Musculoskeletal injuries from Volume 39, No.1, January/February 2010
- Sports related concussion Management in general practice from Volume 39, No.1, January/February 2010
- Sports ankle injuries Assessment and management from Volume 39, No.1, January/February 2010
- Shin pain in athletes Assessment and management from Volume 39, No.1, January/February 2010
- Sports knee injuries Assessment and management from Volume 39, No.1, January/February 2010
- Sport and exercise medicine – a new specialty from Volume 39, No.1, January/February 2010
- AFP in practice from Volume 39, No.1, January/February 2010
- Clinical challenge from Volume 39, No.1, January/February 2010
- Persistent foot pain from Volume 38, No.9, September 2009
- Tendon injuries from Volume 38, No.9, September 2009
- Osteomyelitis from Volume 38, No.7, July 2009
- Upper cervical spine injuries from Volume 38, No.1, January/February 2009







